VIRTUAL VISITS
Improving Care Access, Quality, and Experience
eVisit improves operational efficiencies with a consistent Virtual Visit experience to expand the capacity of care delivery systems and improve health outcomes.



HOW WE HELP
Extending the Reach of Care
Using eVisit, agencies, departments, and programs can deliver care services to service members, veterans, and their families regardless of where they are in the world.

How eVisit Helps Care Delivery Systems Improve Access and Care Quality with Virtual Visits
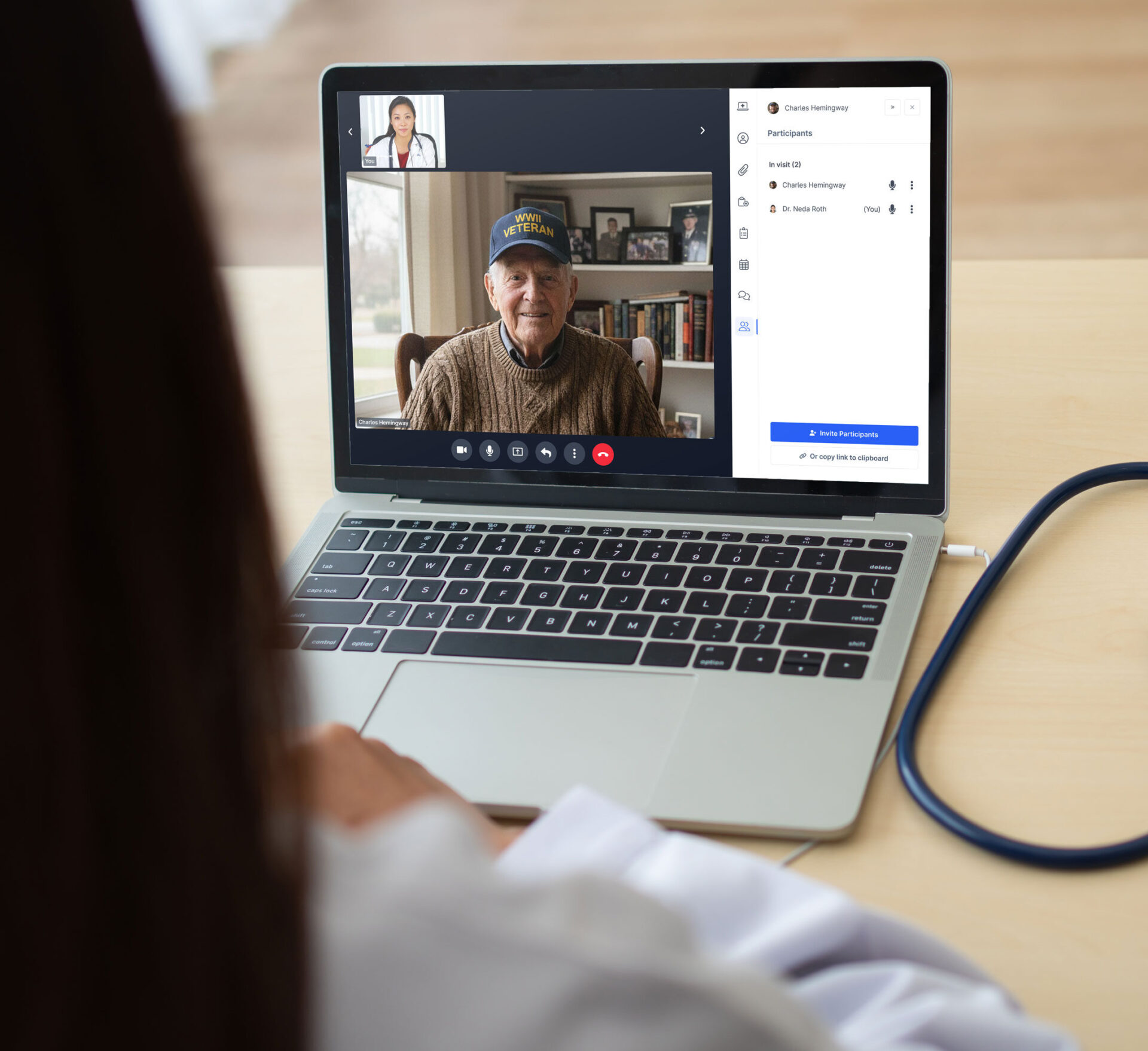
When both the provider and patient are in the Virtual Visit, the clinician can share relevant information in real-time via chat, attachments, documents, or images. When necessary, the provider can also reassign the session to another provider, or add an interpreter, family members, or other clinicians. Providers and patients can also easily schedule the next appointment in real-time during the virtual visit.
Providers can see the patient’s home environment to identify fall risks, other stressors, and can evaluate nutrition needs — which eases the burden of travelling to healthcare facilities to receive care, whether on a military base or VA hospital.