Addressing Workforce Challenges
Improving Caregiver Experiences
Our platform integrates into existing clinical workflows to build better clinician experiences, automate administrative work, and alleviate burdens on the workforce.



HOW WE HELP
Keeping Pace with Evolving Care Team Preferences
By connecting care teams and integrating technology systems to combine digital and in-person workstreams, eVisit improves efficiencies and meets growing expectations for more convenient clinician experiences.

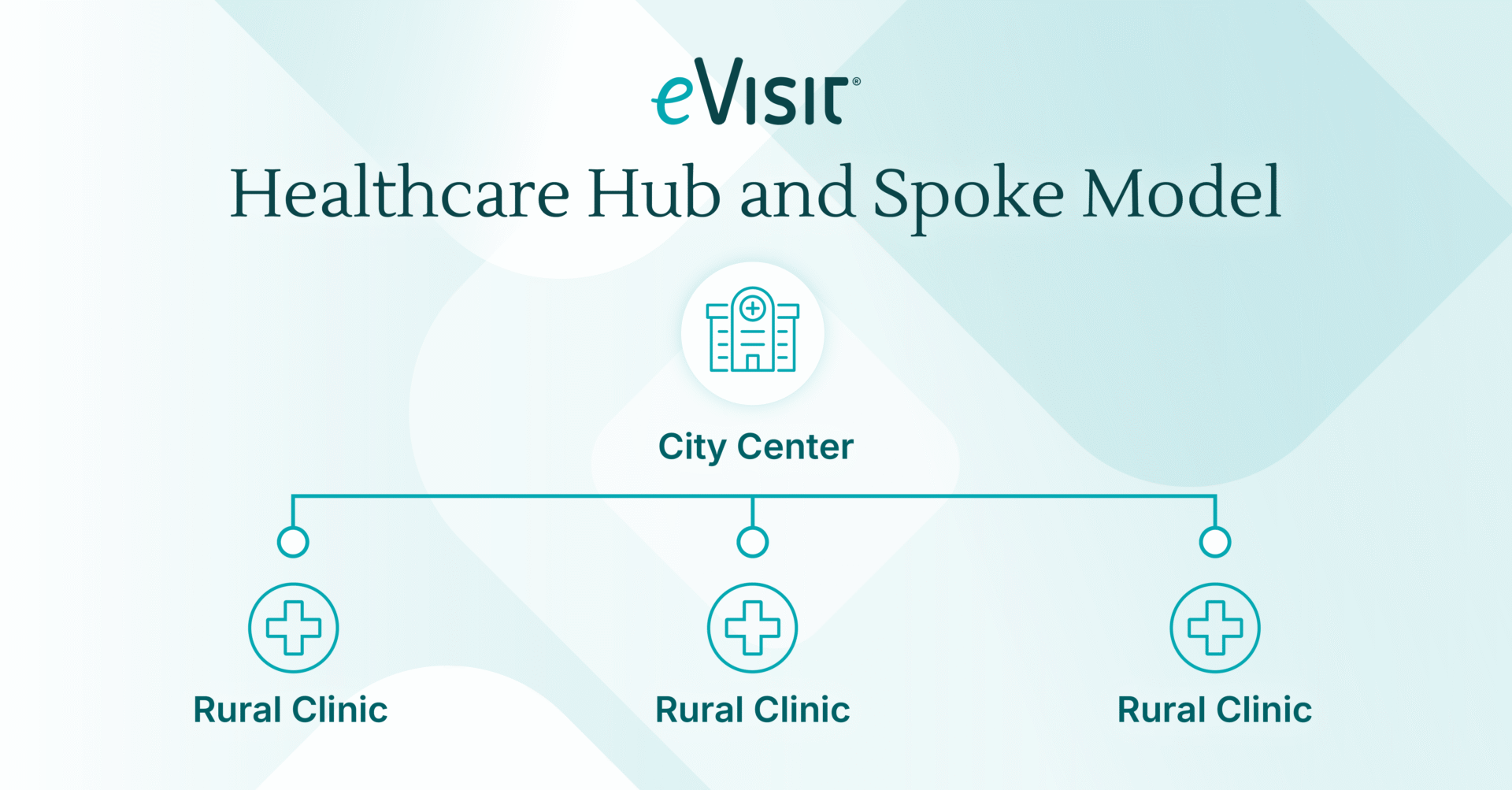
How eVisit Works With Care Delivery Systems to Optimize Staffing
eVisit helps health systems meet evolving care team preferences by enhancing workflows to better suit their needs. Health systems can extend digital work capabilities to clinicians that increase flexibility and enhance work-life balance while drawing on off-site expertise and optimizing labor expenses.
Our platform enables health systems to ease administrative burdens, automate tasks, and improve clinician satisfaction. We elevate clinician experiences by making it easier for care teams to expand access, streamline patient intake and throughput, and manage variability in patient demand—while positively impacting clinical, financial, and operational performance.